Additional Questions?
Please call Billing Customer Service at 1-833-4MYLABS (833-469-5227), available M-F 8AM-7PM ET, or click the link below to contact us today.
CONTACTEste sitio web (y las páginas contenidas) estan desactivado. Si se necesita asistencia en español u otro idioma, por favor llame sin cargas a 800 229 5227.
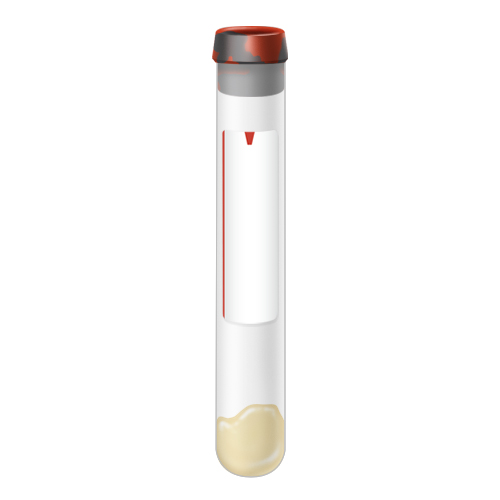
| Code | SST |
|
|---|---|---|
| Name | SST Tube | |
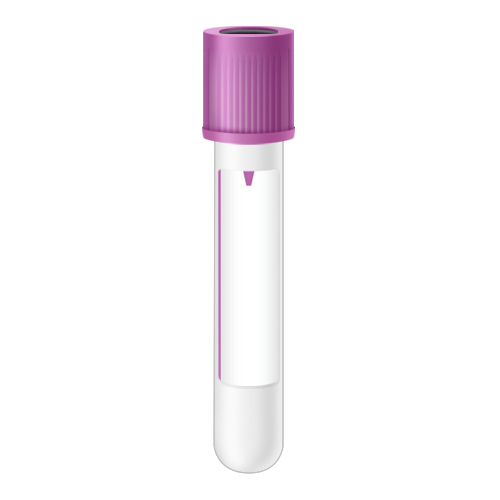
| Code | BML |
|
| Name | Bone Marrow - Lavender Top | |
| Code | LAV |

|
| Name | Lavender top- EDTA | |
| Code | FLUL |

|
| Name | Fluid Lavender (source required) | |
| Code | TAN |

|
| Name | Tan Top | |
| Code | YEL |

|
| Name | Yellow top- ACD | |
| Code | YELS |

|
| Name | Yellow top- SPS | |
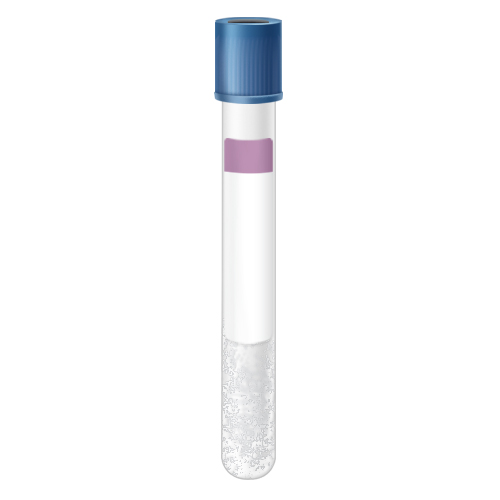
| Code | RBP |
|
| Name | Blue-Royal Blue Top K2 EDTA Plasma(*LAVENDER LINE) | |
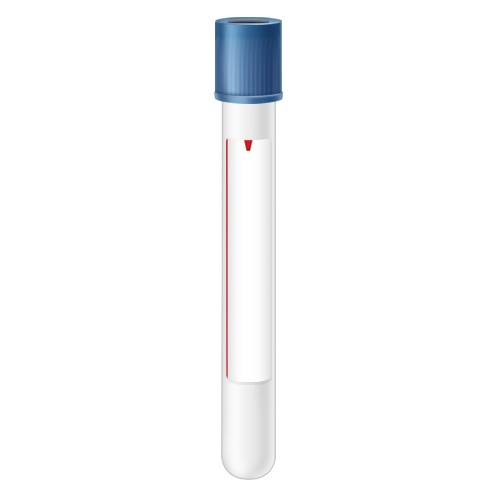
| Code | RBS |
|
| Name | Blue-Royal Blue Trace Element Serum (**RED LINE**) | |
| Code | URB |

|
| Name | Blue-Royal Urine | |
| Code | GRY |

|
| Name | Grey top- Sodium Fluoride | |
| Code | BMG |

|
| Name | Bone Marrow - Green Top | |
| Code | UG |

|
| Name | Green top urine | |
| Code | UGTP |

|
| Name | Green top urine (preservative) | |
| Code | FLUG |

|
| Name | Fluid Green Top | |
| Code | QFT |

|
| Name | Green Top-Lithium Heparin | |
| Code | FLUR |

|
| Name | Fluid Red Top | |
| Code | LTB |

|
| Name | Light blue top | |
| Code | PPT |

|
| Name | White Top (PPT) | |
| Code | ACDNA |

|
| Name | Ariosa Cell-Free DNA (White TopTube) | |
| Code | TP |

|
| Name | ThinPrep Vial | |
| Code | SPTH |
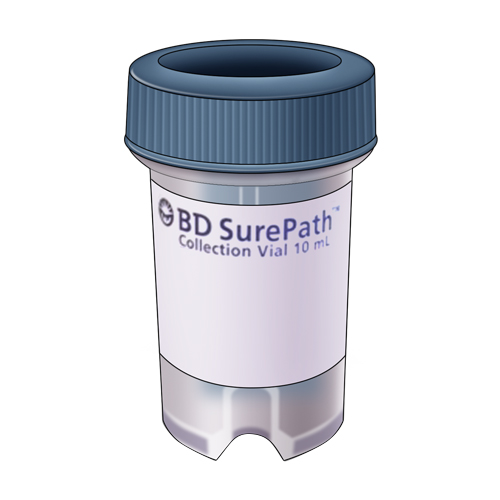
|
| Name | Surepath Vial | |
| Code | O&P |
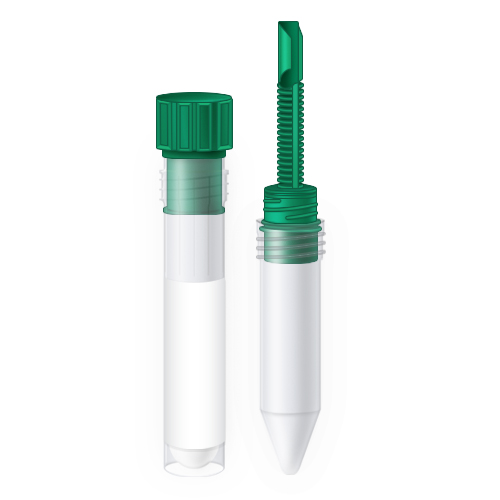
|
| Name | O&P Kit (Total Fix) | |
| Code | U24 |

|
| Name | Urine Container - 24hr | |
| Code | UA |

|
| Name | Urine Urinalysis Tube - Yellow | |
| Code | CUL |

|
| Name | Swab-Bacterial Culture | |
| Code | ES |

|
| Name | Swab-E | |
| Code | APT |

|
| Name | Swab-Aptima Genprobe | |
| Code | UGP |
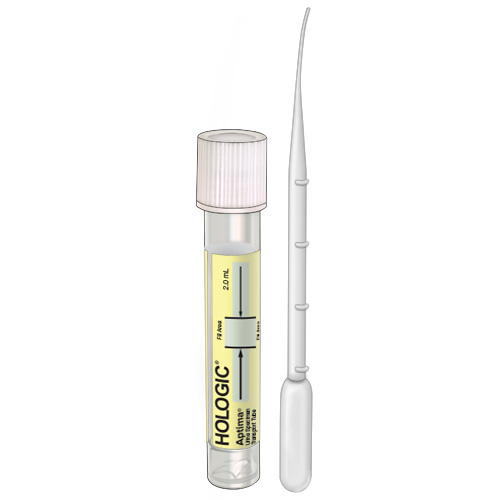
|
| Name | Urine Container-Genprobe-Aptima | |
| Code | BDA |

|
| Name | Affirm(BD) VPIII | |
| Code | RED |

|
| Name | Red Top Plain | |
| Code | UGY |

|
| Name | Urine Tube - Grey Top | |